Knee
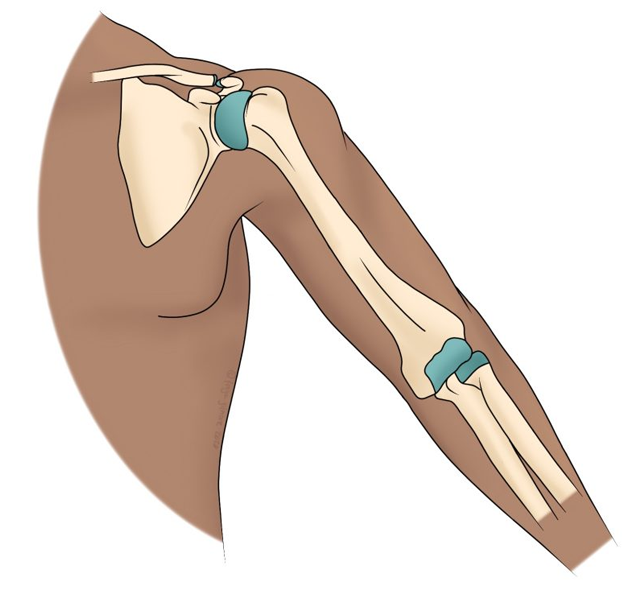
Anatomy
Conditions / Disorders
Procedures
Patellar Dislocations
Patellar dislocation is a painful and distressing event, when the patella jumps clean out of the restraining walls of the groove in which it normally rides.
Patella dislocations are relatively unusual and usually occur in adolescents or young adults. The patella or kneecap usually jumps or runs out of its retaining groove, sometime becoming visible in an abnormal location on the outside of the knee. The injury is associated with significant pain and associated muscle spasm but the dislocation normally reduces when the knee is gently straightened with assistance.
Medical imaging is usually required to exclude the presence of associated fracture or injury to chondral cartilage, and very occasionally the dislocation can be associated with the separation of a fragment of cartilage or bone which falls into the knee joint itself. These injuries are normally treated with a period of splintage followed by rehabilitation supervised by a physiotherapist. Occasionally a kneecap will dislocate on more than one or even several occasions and in these patients patella stabilisation operations are sometimes required.
What happens during a patellar dislocation?
In the first dislocation event the patella usually dislocates to the lateral (outer) side.
This is due to the anatomy of the region. At the same time other structures may be injured, such as the medial patellofemoral ligament which may be torn, and there may also be a small fracture on the medial side of the patella and some associated bone bruising.
Patellar Dislocation: Causes, Symptoms, and Treatment
What is Patellar Dislocation?
Patellar dislocation is a painful and distressing event where the kneecap (patella) moves entirely out of its normal position within the trochlear groove of the femur. This injury often occurs in adolescents and young adults, typically involving the patella dislocating to the outer (lateral) side of the knee. In severe cases, the kneecap may remain visibly displaced.
What Happens During a Patellar Dislocation?
During the dislocation, the patella is forced out of its restraining groove, often resulting in:
- Intense pain
- Significant muscle spasm
- Difficulty bending the knee
The dislocation usually reduces spontaneously when the knee is gently straightened, but professional assistance is often necessary.
What Predisposes to Patellar Dislocation?
Several factors can increase the likelihood of patellar dislocation:
- Anatomical Variations: Conditions like trochlear dysplasia (an abnormally shaped trochlear groove) or patella alta (a high-riding kneecap) can reduce stability.
- Weak or Imbalanced Muscles: Insufficient strength in the quadriceps or other knee-stabilizing muscles.
- Previous Dislocations: Recurrent instability is more likely after an initial event.
Why Can’t I Bend My Knee After a Dislocation?
A dislocated patella is often accompanied by swelling, pain, and muscle spasm, making knee movement difficult. Additionally, associated injuries, such as torn ligaments or loose fragments of cartilage or bone within the joint, can restrict motion.
Can a Dislocated Knee Be Permanent?
While the dislocation itself is rarely permanent, repeated episodes can occur if the underlying structural issues are not addressed. Chronic instability may lead to long-term damage and discomfort, necessitating surgical intervention in severe cases.
Management of Patellar Dislocation
Initial Treatment:
- The dislocation is typically reduced by carefully straightening the knee.
- Medical imaging is performed to rule out fractures, chondral cartilage damage, or loose fragments.
Conservative Management:
- A short period of immobilization with a brace.
- Physiotherapy to strengthen supporting muscles and improve stability.
Surgical Intervention:
- For recurrent dislocations or severe injuries, patellar stabilization procedures may be required. These include reconstructing torn ligaments, realigning the patella, or removing loose fragments from the joint.
If you’ve experienced a patellar dislocation or have concerns about knee instability, schedule a consultation for a comprehensive evaluation and tailored treatment plan.
Braces for Treating Patellar Dislocation
Bracing plays a key role in managing patellar dislocation, particularly in the early stages of recovery or for preventing recurrent dislocations. These devices provide support, stabilize the kneecap, and help restore confidence during movement.
Types of Braces for Patellar Dislocation
- Knee Immobilizers
- Used immediately after the dislocation to keep the knee in a straight position.
- Limits movement to allow healing of injured tissues like the medial patellofemoral ligament (MPFL).
- Patellar Stabilizing Braces
- Designed to maintain proper alignment of the patella within the trochlear groove.
- Often feature lateral buttresses or straps to prevent the kneecap from dislocating outward.
- Used during activities to reduce the risk of recurrent dislocations.
- Dynamic Braces with Hinges
- Provide controlled movement while stabilizing the knee.
- Ideal for patients progressing through rehabilitation who require support during bending and straightening movements.
- Donut Braces
- Feature a circular padding around the kneecap to hold it in place.
- Useful for mild instability and support during physical therapy exercises.
Benefits of Braces in Patellar Dislocation
- Reduces pain and swelling.
- Improves patellar tracking.
- Prevents further injury during recovery.
- Enhances stability during activities and rehabilitation.
Surgical Treatment of Patellar Dislocation
Surgery is considered for patellar dislocation when conservative treatments fail or in cases of recurrent instability, structural abnormalities, or associated injuries such as cartilage damage or loose bone fragments. The primary goal of surgical intervention is to restore stability, prevent further dislocations, and preserve knee function.
Indications for Surgery
- Recurrent patellar dislocations despite physiotherapy and bracing.
- Structural issues such as trochlear dysplasiaor patella alta.
- Damage to the medial patellofemoral ligament (MPFL).
- Loose bone or cartilage fragments in the knee joint.
- Significant impact on the patient’s quality of life or athletic performance.
Surgical Procedures for Patellar Dislocation
- MPFL Reconstruction
- The MPFL, which helps stabilize the patella, is reconstructed using a graft from the patient’s own tissue or a donor.
- This procedure is often the first choice for recurrent dislocations.
- Tibial Tubercle Transfer (TTT)
- The tibial tubercle, where the patellar tendon attaches, is surgically realigned to improve patellar tracking.
- This may involve medialization (shifting inward) or distalization (shifting downward) of the tubercle.
- Trochleoplasty
- Performed in cases of severe trochlear dysplasia, this surgery reshapes the trochlear groove to better accommodate the patella.
- Cartilage Repair or Removal
- Loose fragments of cartilage or bone are removed or repaired during an arthroscopic procedure to restore smooth joint movement.
- Lateral Release and Medial Tightening
- Involves releasing tight lateral structures pulling the patella outward and tightening medial structures to stabilize the kneecap.
Post-Surgical Rehabilitation
- After surgery, patients undergo a structured rehabilitation program with physiotherapy to restore strength, range of motion, and stability.
- Bracing may be used temporarily for support during the healing process.
- Most patients return to daily activities and sports within 4–6 months, depending on the procedure and individual progress.
Expert Care Tailored to You
At COSM we specialize in advanced surgical techniques for patellar dislocation, offering personalized treatment plans to ensure optimal outcomes. Schedule a consultation to discuss your options and take the first step toward a stable, pain-free knee.