Shoulder & Elbow
Anatomy
Conditions / Disorders
Procedures
Total Shoulder Replacement
Shoulder Anatomy
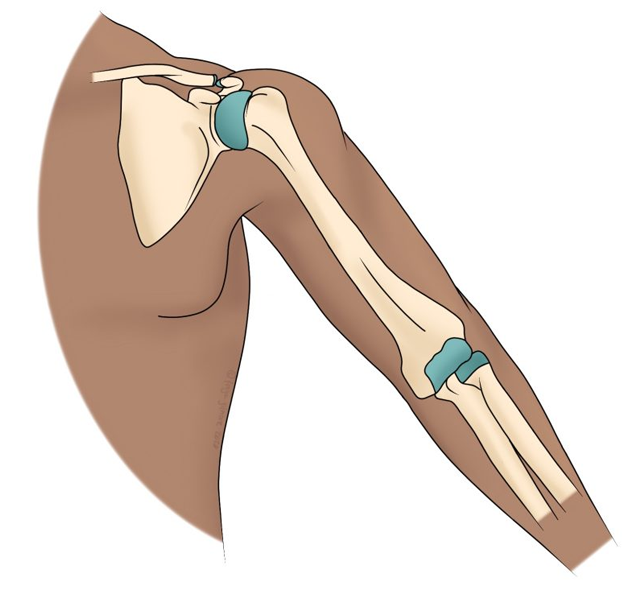
The shoulder is a highly flexible ball-and-socket joint that allows for a wide range of motion in the arm. The head of the humerus (upper arm bone) fits into the glenoid, the shallow socket of the scapula (shoulder blade). Cartilage covers both the humeral head and the glenoid, preventing friction between the bones during movement. Synovial fluid lubricates the joint, and tendons and ligaments around the shoulder provide strength and stability.
What is Osteoarthritis?
Osteoarthritis occurs when the cartilage that cushions the shoulder joint is damaged. As the cartilage wears away, the bones begin to rub directly against each other, resulting in pain, swelling, stiffness, and reduced movement. This condition can severely impact daily activities and quality of life.
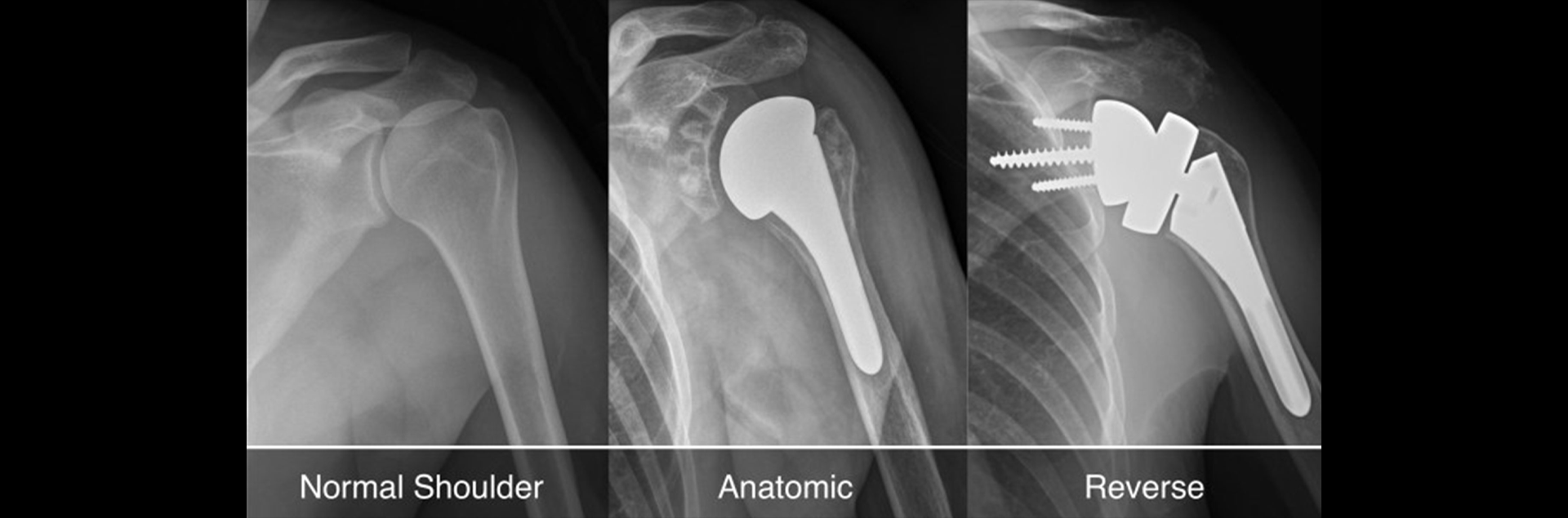
What is Shoulder Joint Replacement?
Total shoulder replacement surgery is designed to relieve the pain and dysfunction caused by osteoarthritis, rheumatoid arthritis, or other degenerative conditions of the shoulder. The procedure involves removing the damaged parts of the shoulder joint and replacing them with artificial components. This includes replacing both the humeral head (ball) and the glenoid (socket) with prosthetic parts. The goal of the surgery is to alleviate pain, improve mobility, and restore function to the shoulder.
Indications for Shoulder Joint Replacement
Total shoulder replacement is recommended for patients who have not found relief from symptoms through non-surgical treatments such as medication, physical therapy, or injections. You may be a candidate for the procedure if you experience:
- Severe shoulder pain that limits your daily activities
- Persistent pain during rest
- Weakness or loss of motion in the shoulder joint
- Reduced ability to perform daily tasks due to shoulder discomfort
Preparation for Shoulder Joint Replacement
Before recommending total shoulder replacement, your surgeon will evaluate your condition through a thorough medical history review, physical examination, and imaging tests such as X-rays or MRI scans. These assessments help determine the extent of damage to the shoulder and the suitability of surgery.
Shoulder Joint Replacement Procedure
The surgery is typically performed under general or regional anesthesia. Depending on your condition and surgeon’s approach, the procedure may be done via:
- Open Surgery: A large incision is made to access the shoulder joint.
- Minimally Invasive Surgery: Small incisions are made to insert an arthroscope (a small camera with a light) and surgical instruments.
The procedure involves the following steps:
- Incision and Exposure: The surgeon makes an incision over the affected shoulder and carefully separates the underlying muscles to reach the shoulder joint.
- Removal of Damaged Tissue: The damaged humeral head (ball) is removed, and the bone is hollowed out to prepare for the prosthetic.
- Humeral Prosthesis: A metal ball with a stem is inserted into the humerus and secured with cement.
- Glenoid Prosthesis: The damaged part of the socket is prepared, and a plastic glenoid component is fixed into the scapula.
- Closing: Once the prosthetic components are in place, the joint capsule is stitched, and the incision is closed.
Post-operative Care for Shoulder Joint Replacement
After surgery, you will be prescribed pain medications and antibiotics to manage discomfort and reduce the risk of infection. You may have your arm placed in a sling or cast to support the shoulder as it heals.
- Rehabilitation: Physical therapy is a key part of recovery and will be initiated shortly after surgery. Therapy helps restore mobility, strength, and function to the shoulder. Gentle daily activities may be resumed within two to six weeks.
- Follow-up: Regular follow-up appointments will be scheduled to monitor recovery and ensure the proper functioning of the prosthetic components.
Risks and Complications of Shoulder Joint Replacement
As with any major surgery, shoulder joint replacement carries some potential risks, including:
- Anesthesia Complications: Nausea, dizziness, or vomiting.
- Infection: There is a risk of infection at the surgical site.
- Dislocation: The prosthetic joint may dislocate, requiring additional surgery.
- Damage to Blood Vessels, Nerves, or Muscles: Though rare, there may be injury to nearby structures.
- Failure to Relieve Pain: The surgery may not achieve the desired pain relief.
- Pulmonary Embolism: A blood clot in the lungs, a serious but rare complication.
- Wear and Tear of Prosthesis: Over time, the prosthetic components may wear out, potentially requiring revision surgery.
Total shoulder replacement can significantly improve the quality of life for individuals suffering from severe shoulder arthritis or injury. For more information or to schedule a consultation with our experienced orthopedic surgeons.